Difference Between Whiteheads, Milia and Fungal Acne
Skin is the largest organ in the body. It envelops and safeguards our bodies. Specific allergies, irritants, cosmetics, or particular illnesses can cause rashes, boils, and other skin conditions. Symptoms like redness, inflammation, stinging, and itching can be brought on by anything that hurts, clogs, or irritates our skin. Some common skin issues, including milia, whiteheads, and fungal acne, may also affect our appearance.
It’s challenging to pinpoint precisely what is wrong with your skin. Could those tiny raised pimples be whiteheads or fungus acne? What exactly is that and what difference does it make? If you need help distinguishing between milia, whiteheads, and fungal acne, keep reading to learn how to diagnose and treat your skin correctly.
Milia
Milia are tiny white bumps that typically develop on the face’s cheeks, nose, and eyes. They may occasionally appear independently, but skin injuries may also cause them. The use of heavy, thick face creams frequently brings on blocked pores and milia.
Milia forms when skin protein is trapped beneath the skin’s surface. It develops when your skin turnover slows down. It is brought on by using heavy, oily cosmetics, such as a face cream that is excessively sticky for you. This allows the keratin to continue to form, and if skin turnover isn’t high enough, it manifests as white bumps.
Symptoms
- Milia are tough, protruding cysts that develop beneath the skin’s epidermis. They range in colour from white to yellowish.
- They can resemble a sand particle or a rigid, milky capsule.
- They typically have a diameter of 1 to 2 millimetres.
- It takes a very long time to disappear and won’t pop.
- They can develop anywhere; however, the face is where they most frequently occur. These could appear around the cheeks, nose, forehead, and eyes.
- Milia are not painful or itchy. They are benign but bothersome.
Treatment
Milia may go away on its own with time, so you may want to let your skin develop naturally. Yet, you may always help your skin by using products like glycolic acid or retinol to speed up cell turnover. Use a cotton ball to apply the product to the troublesome area. Never try to bust it by yourself, as it may further cause harm to your skin and may also leave a scar.
Not every milia will require removal, but let a dermatologist handle the extraction if you choose to do so. In contrast to picking it manually, your doctor can remove it using various techniques like cautery or extractions with the help of tiny blades and sterile needles.
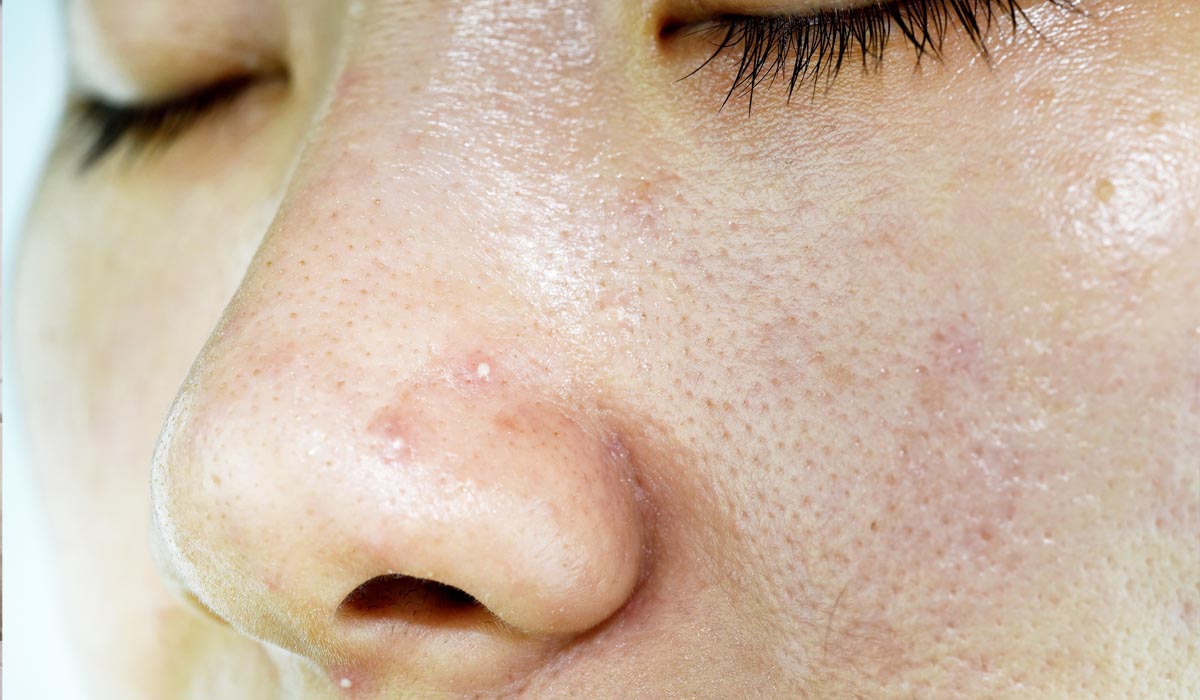
Whiteheads
Whiteheads are more frequently referred to as congested skin because they are located deeper in the skin than blackheads. They resemble tiny, non-inflamed, red pimples under the epidermis. The tiny white head is occasionally visible; other times, it is not. They typically develop on people’s chins, forehead creases, cheeks, and corners of the mouth.
The most common cause of whiteheads is excess sebum generation. When dead skin cells accumulate on the exterior of the pores, obstructing the oil’s discharge, whiteheads appear on the face and the chin. Whiteheads may also be caused by dehydrated skin and using too-heavy or greasy products on your skin.
Symptoms
Whiteheads are simple to identify; some typical symptoms include:
- Whiteheads appear as closed lumps on the skin.
- They are typically yellowish or white in color.
- The face, neck, chest, back, and upper arms are most prone to whiteheads.
- The majority of whiteheads disappear on their own, but it may take some time.
Treatment
Chemical exfoliators such as glycolic acid, lactic acid, mandelic acid, etc., may aid with whiteheads and enhance the skin’s texture. Use a mild aloe mask to properly moisturize the skin if dryness is the cause of the whiteheads.
Everybody’s skin is unique; thus, treatment will vary from person to person. Some techniques and home cure work better for particular skin types and allergies. You should see a skincare expert to determine your skin type and the appropriate at-home cures.
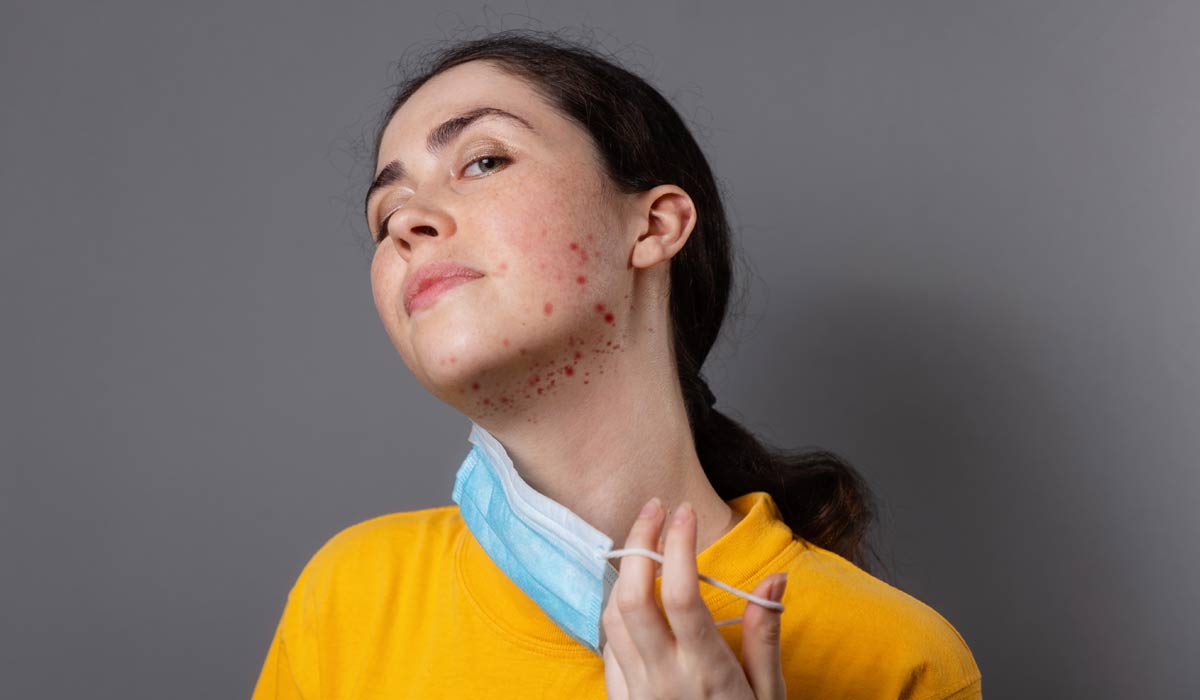
Fungal Acne
Fungal acne is yeast overgrowth or an infection. It is also known as Pityrosporum (Malassezia) folliculitis. Although it can be challenging to self-diagnose fungal acne, it usually itches. These lumps are consistently sized and typically observed in groups. Rows of tiny red bumps resembling fungus can be seen on the temples, cheeks, or, less frequently, the upper chest and back.
The yeast that causes fungal acne is always present in the skin. Typically, the yeast, various fungi, and bacteria, which are also a component of the skin, may be balanced by our body. But if that natural equilibrium is disturbed, an overgrowth could happen. The hair follicles become infected at that point, and acne-like symptoms manifest.
The yeast that promotes acne flourishes in a warm, humid environment. As a result, sweat and sebum may exacerbate fungal acne. A warm and inviting environment for the yeast could be created by over-moisturizing in conjunction with a humid temperature, helping it to flourish and grow even more. Certain oils and cosmetics for the skin, such as avocado and olive oil, may worsen symptoms.
Symptoms
In appearance, fungal acne resembles acne vulgaris, or bacterial acne, which is one of the reasons why it can persist for a long time. Here’s how to identify fungal acne:
- Fungal acne typically results in pus-filled pimples.
- It frequently manifests on the back, chest, and arms. It can also occur on the face, where bacterial acne typically occurs.
- Itching is a common side effect of fungus acne.
- Little whitehead clusters are a standard feature of fungus-induced acne.
Treatment
Fungal acne can be treated with anti-acne gel. As fungal acne is challenging to treat with antibiotics, you should remove all harmful components from your beauty products. It would help to reestablish the correct ratio of bacteria and yeast on the skin to treat the fungal infection effectively. See a dermatologist if you’ve tried home remedies for your suspected fungal acne and the outbreak lasts longer than 3 weeks.
Why choose 7DMC?
We provide exceptional medical and aesthetic solutions to meet your cosmetic requirements. Under the skilled guidance of our outstanding medical staff, we use the most sophisticated, cutting-edge equipment. Our doctors have unique clinical backgrounds and exceptional academic records. Our mission is to provide the best-individualized patient care possible. We adopt a patient-centered strategy to provide a treatment plan based on your requirements, lifestyle, and objectives.
Bottom Line
We are susceptible to hundreds of different skin problems. Learning what characteristics to look out for can be crucial, as some of the most common conditions may have similar symptoms to others. While some skin disorders are not harmful, some can have symptoms, including discomfort and irritation. It’s critical to remember that nobody should struggle with skin problems by themselves. Working with a dermatologist can ensure a proper diagnosis and the best course of action.
References:
healthline.com/health/all-about-fungal-acne
verywellhealth.com/description-of-millia-15572
medicalnewstoday.com/articles/315104