A Clinical Approach to Treating Pelvic Floor Disorders
Pelvic floor disorder is one of the most common illnesses mainly found in females. Data shows that at least 1/3rd of the female population eventually suffer from pelvic floor dysfunction. As females age, pelvic floor muscle dysfunction begins.
What is pelvic floor disorder?
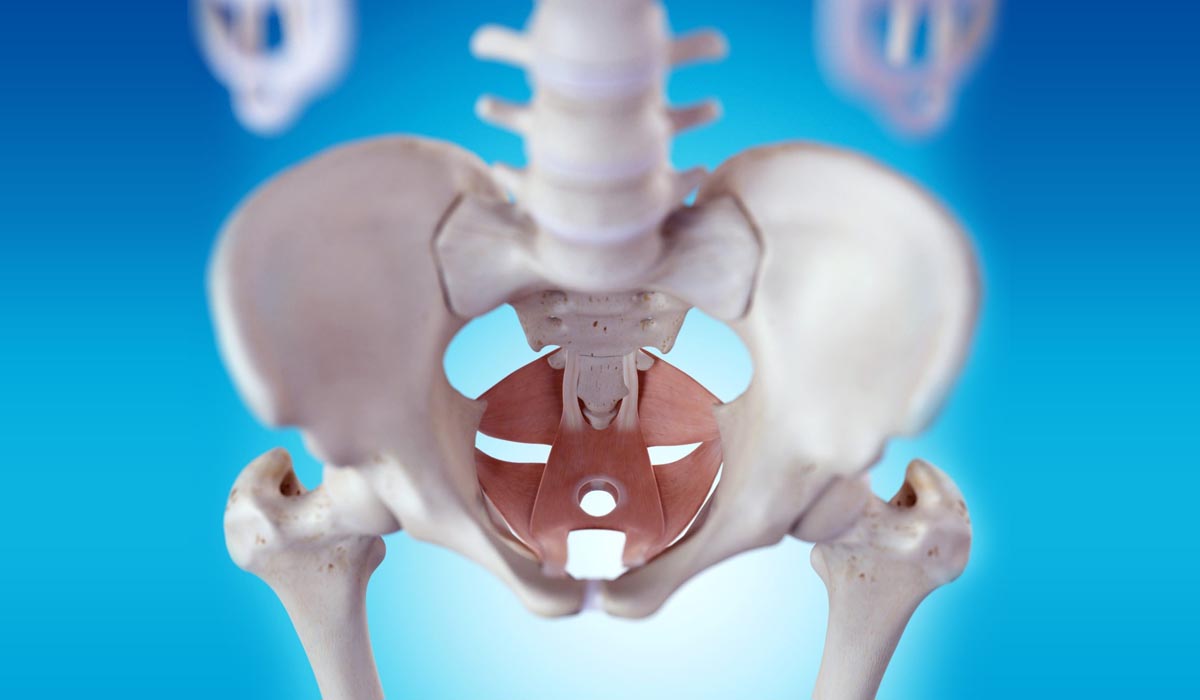
The pelvic floor is a network of muscles and tissues that acts as a hammock to hold the uterus, cervix, vagina, bladder, bowel, urethra, small intestine, and rectum. When these pelvic muscles strain due to tear or loosening, the disorder occurs.
Aged people, particularly females, with the deterioration of the body and who’ve given natural birth, are more likely to suffer from the pelvic floor disorder.
Types of Pelvic Floor Disorder
There are mainly two categories in which the Pelvic Floor Disorder can be classified. One, where the tissues protrude abnormally outside the body. Second where the muscles start functioning abnormally and cause irritations.
The 1st types are:
- Vaginal or rectal prolapse (sagging of the vagina or rectum)
- Rectocele (protrusion or herniation of the rectum into the vagina)
- Cystocele (a herniation of the bladder into the vagina)
- Enterocele (a herniation of the intestine into the vagina)
- Sigmoidocele (a herniation of the sigmoid colon into the vagina)
- Post-operative pelvic floor hernias
The 2nd types are:
- Urinary incontinence
- Faecal incontinence
- Constipation
- Sexual dysfunction
- Low anterior resection syndrome (occurs most often after rectal cancer surgery)
Let’s look in details at each type:
Often there are many organs of the pelvic region that get affected. The organs fall out of their place and hang outside the body through the vagina majorly.
Pelvic organ prolapse types include:
Rectocele – here the rectum sticks out through the back wall of the vagina
Cystocele – where the bladder sticks out through the anterior vaginal wall
Sigmoidocele – refers to a condition where the sigmoid colon prolapses into the lower pelvic cavity.
Enterocele – the small intestine protrudes into the lower pelvic cavity.
Vaginal vault prolapse or uterine prolapse occurs when the entire vagina or uterus sag through the vaginal opening.
Rectal prolapse occurs when the lining and/or muscles of the rectum slips out of the anus.
Also, in certain cases, the organ may slip out of the original location but not necessarily, out of the body. Unless it comes out hanging from some orifice, patients may not even recognise the misplacement of the organs.
The 2nd types where there is no prolapse are:
Urinary incontinence
This condition arises mainly after childbirth in females. The pelvic muscles loosen and may not remain capable of holding the bladder. Hence the bladder slips out of its place and pushes against the vagina, causing the urethra muscles to force open.
Faecal incontinence
Faecal incontinence is the inability to control bowel movements, causing stool (faeces) to leak unexpectedly from the rectum. It mainly happens in females with obstetric injuries or in males, who may have undergone rectal cancer surgeries or anal sphincter trauma.
Constipation
Constipation is another pelvic floor condition that may not respond to laxatives or oral constipation medications. This may be triggered due to some internal pelvic floor obstruction.
Sexual dysfunction
The symptoms may include reduced sexual arousal, infrequent orgasm or dyspareunia in females. Erectile dysfunction may be related to limited arterial blood flow in males, suffering from Pelvic floor disfunction.
Low anterior resection syndrome
People may suffer from this syndrome mainly after surgery to resect or remove part of or the entire rectum. The surgery may be related to rectal cancer.
Pelvic floor dysfunction treatment options
Getting help and recovering from pelvic floor disorder in the modern times has become easier. In earlier days, the issues related to urinary incontinence or sexual dysfunction, which were seen as a part of ageing, are getting recognised and dealt with comprehensive clinical treatments now.
They can be treated non-surgically, and the treatments includes:
Biofeedback
This is the most common form of treatment available. It is done with the help of physical therapist and helps more than 75% of the cases of patients suffering from pelvic floor malfunction. The therapist may monitor and retrain the muscles to bring them in their original positions. They may ask you to clench or relax the muscles in a way to boost the strength of the tissues and the ligaments. It is the best non-painful technique of pelvic floor treatment.
Pelvic floor physical therapy
Pelvic floor physical therapy is simultaneously done with Biofeedback therapy. In this the therapist recognises which muscles in your lower back, pelvis and pelvic floor can be strengthen and stretched, that can support the whole network of pelvic muscle area. This eventually increases the coordination between the pelvic floor.
Medications
Laxatives and stool softeners are commonly prescribed by your gastroenterologist to keep the bowel movement smooth. These can help improve the dysfunction and may cure it slowly.
Relaxation techniques like meditation can also help. Warm bath, yoga and exercising, coupled with nutritional diet, can go a long way in the treatment of pelvic floor disorders.
Other minor invasive surgical techniques are also available. These includes:
Synthetic and Biological Graft Materials for Pelvic Floor Reconstructive Surgery
After the FDA cleared the use of surgical mesh products, specifically for stress urinary incontinence (SUI) in 1996 and pelvic organ prolapse (POP) in 2002, there has been a spurt of synthetic and biological mesh usage in reconstructive surgeries. Transvaginal mesh implants for POP, although, is no longer suggested because report shows that it has led to other complications such as pain, infection, bleeding, dyspareunia, organ perforation, and urinary problems.
Biological grafts, which are better alternatives of synthetic mesh, has been used since 100 plus years with high efficacy in treatment of SUI.
Pelvic Organ Prolapse Reconstructive Surgery
There are mainly two types of Prolapse Reconstructive Surgeries.
- Obliterative surgery
- Reconstruction
- Obliterative surgery – Colpocleisis is a type of obliterative surgery where the front and back walls of the vagina is sewn together. This prevents the vaginal walls to stick out and provide support to the internal organs.
- Reconstruction surgeries are performed when non-invasive procedure proves futile. There are various reconstruction procedures for correcting various pelvic organ prolapse, such as bladder, rectal, uterine or vaginal.
Stress Urinary Incontinence Surgery
Colposuspension is a type of surgery which involves making a cut in the lower abdomen and lifting the tip of the bladder and stitching it in this way.
Faecal Incontinence Surgery
Injecting biomaterial in the anal canal helping it bulk up and squeeze the anas is a process of surgery for faecal reconstruction.
Another method is repair of sphincter muscles (sphincteroplasty). The most common cause of sphincter muscles is childbirth.
In Overlapping sphincteroplasty, an electrical lead is placed within the sacrum to simulate the nerves. The nerves are simulated by a nerve simulator, which functions similar to a heart pace maker. This procedure is done in phased manner. At first, the lead is placed within the sacrum and the wires are placed outside. The patient keeps a diary of the bowel habits, and if the recovery is more than 50%, than a permanent nerve simulator is placed under the buttock skin.
Conclusion
Pelvic floor disorder can be a debilitating condition having a wide variety of causes. There are various techniques to treat this disorder which includes non-surgical as well as surgical methods. A through clinical investigation can reveal the exact cause of the disorder and eventually a treatment process can be undertaken. Depending on the severity of the disorder, treatment can be done by a physical therapist, a gynaecologists, a gastroenterologist, a pelvic pain anaesthesiologists, or a pelvic floor surgeon.
Ref:
https://www.tanner.org/the-scope/a-clinical-approach-to-treating-pelvic-floor-disorders
https://my.clevelandclinic.org/health/diseases/14459-pelvic-floor-dysfunction/management-and-treatment
https://www.massgeneral.org/pelvic-floor/treatments-and-services/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6849106/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3498251/
https://fascrs.org/patients/diseases-and-conditions/a-z/fecal-incontinence-expanded
https://medlineplus.gov/ency/article/007376.htm#:~:text=Vaginal%20sling%20procedures%20are%20types,your%20urethra%20and%20bladder%20neck.
https://www.healthline.com/health/womens-health/colpocleisis
https://www.acog.org/womens-health/faqs/surgery-for-pelvic-organ-prolapse